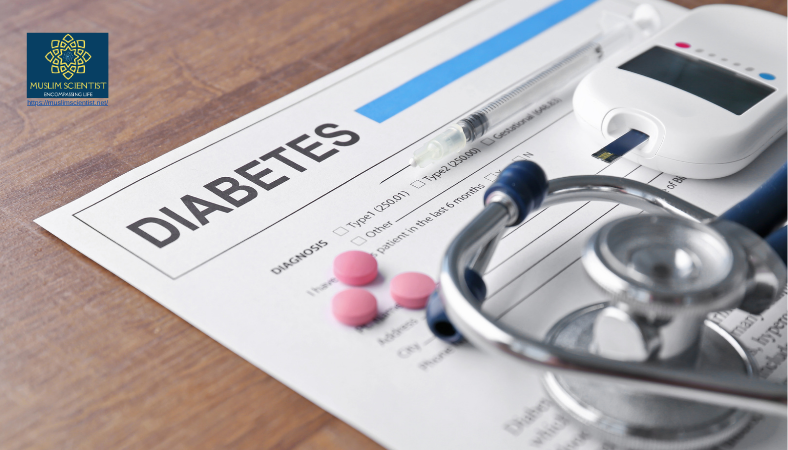
There are millions of Muslims living in the United States. For them, the holy month of Ramadan is a time of profound spiritual connection, community, and fasting from dawn to sunset. But for the estimated 150 million Muslims worldwide living with diabetes, this sacred practice presents a complex challenge: how to fulfill a religious obligation while safely managing a chronic condition that requires regular meals and medication.
A study from the University of Memphis, published in the journal Diabetology, offers unprecedented insights and encouragement. By listening directly to the voices of Muslim Americans with Type 2 diabetes, the research illuminates not only the struggles but also the immense opportunity that Ramadan presents for making sustainable, positive lifestyle changes. It is one of the first studies to deeply explore the dietary behaviors and psychosocial factors of this community within the US context.
The Hidden Challenge: Fasting in a Non-Muslim Majority Country
The United States is home to a vibrant and diverse Muslim population of about 3.45 million, hailing from South Asia, the Middle East, North Africa, Somalia, and beyond. Many of these communities also face a disproportionately high risk of diabetes. For example, South Asians, who make up a significant portion of US Muslims, have a diabetes prevalence of 26.7%—far higher than the general population.
During Ramadan, adult Muslims abstain from all food and drink from dawn to sunset. Islamic law provides exemptions for people who are ill, including those with chronic conditions like diabetes, for whom fasting could pose a health risk. However, many choose to fast for deeply personal reasons: to gain spiritual rewards, to feel a sense of normalcy with family and friends, and to participate fully in the communal aspect of the month.
Previous international studies have shown that fasting during Ramadan can increase the risk of severe hypoglycemic (low blood sugar) and hyperglycemic (high blood sugar) events. Compounding this, many Muslim patients are reluctant to discuss their fasting plans with their healthcare providers, fearing that non-Muslim doctors may not understand or support their religious practice. This communication gap can leave patients navigating the month without proper medical guidance.
The Study: Giving Voice to the Community
To bridge this gap, a research team led by Dr. [Lead Researcher’s Name, if available, otherwise use “The research team”] at the University of Memphis employed a community-engaged approach. They conducted in-depth, one-on-one interviews with 22 Muslim adults living with Type 2 diabetes from five diverse US communities, including individuals of Arab, South Asian, Somali, Afghan, and African American backgrounds. This qualitative method allowed participants to share their experiences, struggles, and successes in their own words.
The goal was to understand, from the patient’s perspective:
- How their dietary habits change during Ramadan.
- The key personal, social, and cultural factors influencing those changes.
- How these factors ultimately affect their diabetes control and health.
The Encouraging Findings: More Than Just a Fast
The analysis revealed six main themes, painting a rich picture of the Ramadan experience. Two key findings stand out as particularly encouraging for patients and healthcare providers.
First, the study confirmed that Ramadan is a time of significant dietary change. Participants described shifting to eating two main meals—one before dawn (Suhoor) and one after sunset (Iftar)—often with a focus on traditional, festive foods. This change, while challenging, creates a natural “intervention period” where old habits are paused, and new ones can be formed.
Second, and most importantly, the study found that many participants viewed Ramadan not as a burden, but as a powerful opportunity for positive, sustainable change. They reported that the structure and spiritual focus of the month helped them reset their relationship with food, increase self-discipline, and even lose weight. Some expressed a desire to continue healthier eating patterns long after Ramadan ended.
Table 1: Key Dietary and Psychosocial Themes from US Muslims with Diabetes During Ramadan
This table summarizes the main themes identified in the study, highlighting both the challenges and the opportunities.
| Theme | Description | Implication for Health |
|---|---|---|
| Change in Dietary Habits | Shift to two main meals (Suhoor & Iftar); increased consumption of traditional fried and sugary foods at Iftar. | Increased risk of hyperglycemia if not managed. Opportunity to plan balanced meals. |
| Influence of Social & Cultural Practices | Strong pressure to participate in large communal meals; difficulty saying no to food offered by family. | Can lead to overeating. Highlights need for family support and education. |
| Variable Self-Efficacy | Confidence in managing diet fluctuates; some feel in control, others feel overwhelmed. | Indicates a need for tailored support to build confidence. |
| Learning from Health Outcomes | Experiences of hypoglycemia or hyperglycemia directly inform next-day food choices (e.g., reducing sweets after a high reading). | Patients are actively learning; this is a key moment for provider guidance. |
| Ramadan as an Opportunity | Many view the month as a chance to reset habits, lose weight, and practice self-discipline. | A powerful motivator for sustainable long-term change. |
The researchers also examined the specific foods and behaviors that impacted blood sugar. The table below illustrates some of the common dietary patterns reported and their potential effects.
Table 2: Common Dietary Behaviors During Ramadan and Their Impact on Diabetes
| Behavior | Typical Timing | Potential Impact on Blood Sugar |
|---|---|---|
| Consuming sugary drinks & fried snacks | At Iftar (breaking the fast) | Rapid spike in blood sugar (hyperglycemia) |
| Eating large, carbohydrate-heavy meals | At Iftar or late evening | Prolonged elevation of blood sugar |
| Skipping the pre-dawn meal (Suhoor) | Before dawn | Increased risk of low blood sugar (hypoglycemia) during the day |
| Drinking insufficient water | During non-fasting hours | Risk of dehydration, which can affect blood viscosity and kidney function |
| Mindful eating & portion control | Throughout the night | Better blood sugar stability and weight management |
What This Means for Patients and Doctors
This research provides a clear roadmap for improving diabetes care for American Muslims. It highlights that effective support must go beyond simply handing out a diet sheet. It must be culturally tailored and acknowledge the profound role of faith and community.
For patients and families, the message is one of empowerment. The study confirms that your experiences matter and that your desire to fast is valid. It encourages you to:
- Plan ahead: Work with your healthcare provider before Ramadan to adjust medication timing and create a meal plan.
- Focus on Suhoor: Don’t skip this crucial pre-dawn meal. Include complex carbohydrates and protein for sustained energy.
- Be mindful at Iftar: Start with dates and water, as is traditional, but then choose a balanced meal and avoid overeating fried and sugary foods.
- Involve your family: Share what you’ve learned about healthy eating so your loved ones can support you.
For healthcare providers, the study is a call to action to become “culturally competent.” This means:
- Initiating the conversation: Ask your Muslim patients with diabetes about their plans for Ramadan well in advance.
- Listening without judgment: Understand that for many, fasting is a deep spiritual commitment.
- Providing practical, tailored advice: Help patients navigate the dietary changes, adjust medications safely, and recognize warning signs.
- Seeing the opportunity: Recognize that Ramadan can be a “teachable moment” to motivate patients toward long-term health goals.
Conclusion: A Path Forward
This landmark study from the University of Memphis does more than just document challenges; it shines a light on a path forward. By centering the voices and experiences of US Muslims with diabetes, it reveals that with the right support, the holy month of Ramadan can be transformed from a period of health risk into a powerful catalyst for sustainable well-being. It is a testament to the importance of culturally sensitive, patient-centered care—care that sees the whole person, including their faith, as a source of strength.
Reference: here
Other Articles: