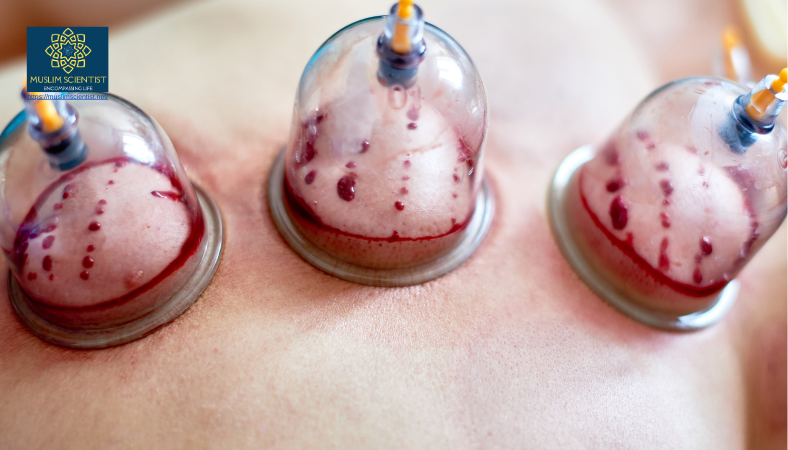
A pilot study from Saudi Arabia explores hijama (wet cupping) as a potential adjuvant therapy, showing significant reductions in harmful antibodies and improved thyroid vitality in patients with this chronic condition.
For millions living with Hashimoto’s thyroiditis, an autoimmune disease where the body’s immune system attacks the thyroid gland, management often means a lifelong reliance on thyroid hormone replacement medication. While essential, this treatment addresses the symptom—hormone deficiency—but not the underlying autoimmune fire. Now, a pilot controlled study published in Saudi Medical Journal offers a glimmer of hope for a more holistic approach, investigating an ancient therapy known as wet cupping, or hijama.
The research, conducted at King Abdulaziz University Hospital in Jeddah, provides preliminary but encouraging evidence that hijama may help modulate the misguided immune activity at the heart of Hashimoto’s, potentially improving gland function and reducing inflammation.
Understanding Hashimoto’s and the Study’s Goal
Hashimoto’s disease is the most common cause of hypothyroidism. It occurs when the immune system produces antibodies that target thyroid proteins, specifically Thyroid Peroxidase (TPO) and Thyroglobulin (TG). This leads to chronic inflammation, gradual destruction of thyroid tissue, and an underactive gland. Patients often struggle with fatigue, weight gain, brain fog, and a host of other symptoms.
The study’s primary objective was bold: to see if hijama—a traditional therapy involving gentle suction and minimal skin incisions to draw out small amounts of blood from specific points—could influence these autoimmune markers and improve patients’ thyroid profiles.
The Study Design: A Controlled Pilot
The research team enrolled 13 adult female patients with Hashimoto’s, all of whom were on stable, conventional thyroxine medication. This “intervention group” underwent three hijama sessions at three-week intervals. A control group of another 13 patients continued with their usual care.
The hijama was applied to anatomical locations theorized to be involved in the immune and disease process: near the thyroid gland, at the sternal angle (targeting areas linked to immune cell development), and near enlarged lymph nodes.
Researchers measured key blood markers before and after the intervention, including anti-TPO and anti-TG antibodies (the primary indicators of autoimmune attack), Thyroid Stimulating Hormone (TSH), thyroid hormones, and Erythrocyte Sedimentation Rate (ESR—a marker of general inflammation).
The Findings: Significant and Encouraging Shifts
The results, while from a small pilot study, were statistically significant and pointed in a promising direction.
1. Reduction in Autoimmune Attack: The most crucial finding was a significant decrease in the levels of harmful anti-thyroid antibodies in the hijama group, while the control group saw an increase.
- Anti-TG antibodies plummeted by an average of 229.06 IU/ml in the hijama group but increased by 28.39 IU/ml in the control group.
- Anti-TPO antibodies also decreased by an average of 60.47 IU/ml with hijama, compared to a rise of nearly 99 IU/ml in the control group.
This suggests hijama may help calm the specific immune response attacking the thyroid.
Table 1: Impact of Hijama on Key Thyroid Autoantibodies
| Marker & Group | Baseline Level (Mean) | Level After 3 Sessions (Mean) | Mean Change |
|---|---|---|---|
| Anti-TG (Hijama Group) | 314.06 IU/ml | 84.99 IU/ml | -229.06 IU/ml (Decrease) |
| Anti-TG (Control Group) | 199.09 IU/ml | 227.48 IU/ml | +28.39 IU/ml (Increase) |
| Anti-TPO (Hijama Group) | 153.00 IU/ml | 86.20 IU/ml | -60.47 IU/ml (Decrease) |
| Anti-TPO (Control Group) | 301.93 IU/ml | 397.76 IU/ml | +98.95 IU/ml (Increase) |
2. Improved Thyroid Function and Reduced Inflammation: Despite patients maintaining the exact same dose of thyroid medication throughout the study, their TSH levels (which should be lower with adequate treatment) decreased significantly. This indicates an intrinsic improvement in the thyroid gland’s own function or hormone utilization. The inflammation marker ESR also dropped.
3. Morphological Improvements on Ultrasound: Thyroid ultrasound scans revealed tangible physical improvements:
- Size & Vascularity: Out of 9 patients with abnormal blood flow in the thyroid, 7 showed improvement. Some with enlarged glands saw a reduction in size.
- Lymph Nodes: 5 out of 9 patients with enlarged cervical lymph nodes returned to normal appearance after therapy.
4. Patient-Reported Symptom Relief: Perhaps most importantly, patients themselves reported substantial improvements. Many experienced 50-100% relief in common hypothyroid symptoms like constipation, irregular periods, low energy, poor concentration, and sleep disturbances.
Table 2: Patient-Reported Clinical Improvement After Hijama
| Symptom | Percentage of Patients Reporting 50-100% Improvement |
|---|---|
| Constipation | High Incidence |
| Period Regularity | High Incidence |
| Energy Level | High Incidence |
| Concentration Ability | High Incidence |
| Sleep Quality | High Incidence |
How Could This Work? Proposed Mechanisms
The study authors propose several theories for these effects:
- Direct “Detoxification”: The suction may help remove inflammatory mediators (like cytokines), autoantibodies, and even heavy metals (linked to autoimmunity) from the interstitial fluid and capillaries around the treated areas.
- Enhanced Blood Flow & Clearance: The therapy may induce localized hyperemia, improving circulation and accelerating the clearance of inflammatory substances from the thyroid region.
- Immune System Modulation: By targeting areas near the sternum (linked to thymus and bone marrow function), hijama might influence the sites where immune cell education and tolerance occur.
A Note of Cautious Optimism and Future Directions
The researchers are clear: this is a pilot study with limitations, including a small sample size. It is not conclusive proof, but a strong signal justifying larger, more robust clinical trials.
“Findings from this pilot study support the hypothesis of hijama efficacy in modulating autoimmune and inflammatory activity of HD and enhancing thyroid function,” the authors conclude. They emphasize the need for further prospective controlled trials with adequate design and sample size.
For the global Hashimoto’s community, this research opens a new, integrative avenue for exploration. It suggests that adjuvant therapies targeting inflammation and immune modulation, like hijama, could potentially work alongside conventional medicine to not just manage symptoms, but possibly alter the disease course itself—offering a new layer of hope for long-term wellness.
Reference: here
Other Articles: